PVD - Peripheral Vascular Disease
The term peripheral vascular disease is commonly referred to as a collection of diseases of the circulatory system, any disorder that affects blood vessels.

Peripheral Artery Disease affects approximately 21 million people in the U.S. and is projected to rise to over 24 million by 2030¹¹

Critical Limb Ischemia affects up to 3.4 million Americans¹¹ with approximately 40% of those requiring an amputation within 6 months of diagnosis.¹²

Deep Vein Thrombosis affects approximately 900,000 people in the United States annually. More than 50% of those diagnosed will have long-term complications.²

Deep Venous Disease Up to 40% of people in the United States have DVD. It occurs more frequently in people over age 50, and more often in women than in men.⁶

Superficial Venous Insufficiency affects between 30-50% of the adult population making it one of the most prevalent causes of venous disease in United States.⁵
PVD Symptoms
Have you experienced any of these?
While some patients with PVD have very few symptoms, others may experience one or more symptoms depending on the disease progression.1 These symptoms can include: spider, reticular, or varicose veins, swelling, skin changes, tired heavy legs, pain with exercise, pain at rest or non-healing wounds. Consult your doctor right away if you have signs of PVD.
Symptoms of PVD

PVD Categories & Conditions
Peripheral Vascular Disease (PVD) is a complex disease which affects the anatomy and physiology of the legs. During diagnosis, a physician will try to assess the cause and extent of damage to the peripheral system. Conditions may occur singularly or in a combination.
Common PVD Conditions8
Learn more about the most common PVD conditions which vary in progression, symptoms, diagnostics and treatment. Find out when to call a doctor and how patients are living with PVD today.
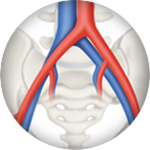
Artery Disease
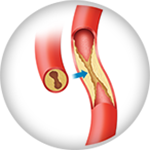
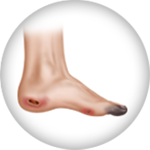
Clotting Disorders
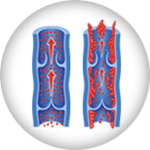
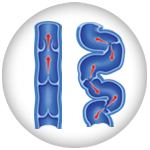
Venous Disease
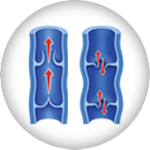
Deep Venous Insufficiency
Lymphedema
Lymphedema is a condition that affects the lymphatic vessels. This results in swelling as fluid pools in the legs and feet. CVI diminishes the capacity of the venous system and it increases the workload for the lymphatic system in the affected area.10
PVD & Me: Patient Stories
Read the inspiring stories of real patients with various conditions of PVD. Learn about their diagnosis, treatment and journey to regaining their quality of life.
PAD Stories
DVD Stories

Patients with deep venous disease (DVD) often go through years of suffering with worsening symptoms and other underlying conditions. Learn about Melanie’s path to uncovering an underlying condition and her road back to restore her health.
DVT Stories

Deep vein thrombosis (DVT) can strike quickly with little notice. Learn more about Reid’s condition and his road to recovery.
CLI Stories

Early intervention can be key for critical limb ischemia (CLI). Learn about Mark’s struggles and triumph to overcome CLI.
Helpful Resources

PVD Doctor
Discussion Guide
Get helpful tips and advice on how to talk to your doctor about a PVD screening.

Patient Brochures
Third-Party Resources
Helpful Websites
Blogs
Apps
A mobile app built by cardiologists, to simplify understanding of most cardiac and peripheral vascular conditions and treatments.
Find a Doctor that Treats PVD
Consult your doctor to learn more about PVD and how to maintain your health. You can also use our Doctor Finder tool below to find a specialist near you.
This tool is not inclusive of all specialists. Consult with your insurance provider to find specialists that are covered within your network.
Are You a Healthcare Professional?
Find out how to register your practice with us.
1. “Peripheral Artery Disease (PAD) Fact Sheet.” Centers for Disease Control and Prevention. June 16, 2016 2. “Venous Thromboembolism (Blood Clots).” Centers for Disease Control and Prevention. August 13, 2015 3. Teraa et al. “Critical Limb Ischemia: Current Trends and Future Directions.” J. American Heart Association. Feb. 23, 2016 4. “Facts about Peripheral Artery Disease (PAD).” National Institutes of Health. Publication No. 06-5837, August 2006. 5. D Carradice. “Superficial venous insufficiency from the infernal to the endothermic.” Ann R Coll Surg Engl. 2014 Jan; 96(1): 5–10. 6. “Chronic Venous Insufficiency.” Cleveland Clinic. 12/15. 7. “Peripheral Artery Disease (PAD).” Mayo Clinic. Aug. 12, 2017 8. “Understand Your Risk for PAD.” American Heart Association, n.d. 9. “Peripheral Vascular Disease(PVD).” Stanford Health Care (SHC) – Stanford Medical Center. 13 July 2016 10. Melissa Conrad Stöppler. “Lymphedema.” MedicineNet.com. n.d. 11. Yost M. Critical Limb Ischemia Volume I, United States Epidemiology, Supplement 2016. Atlanta, GA: The Sage Group; 2016.HCUP Nationwide Inpatient Sample (NIS). Healthcare Cost and Utilization Project (HCUP). Rockville, MD: Agency for Healthcare Research and Quality; 2009 12. “Reducing Amputation Rates in Critical Limb Ischemia Patients Via a Limb Salvage Program: A Retrospective Analysis” Vascular Disease Management, May 2016. Disclaimer The opinions and clinical experiences presented herein are for informational purposes only. Individual results may vary depending on a variety of patient-specific attributes and related factors. Dr. Raghu Kolluri has been compensated by Philips for his services in preparing and providing this material for Philips further use and distribution. We offer links to third-party websites that may be of interest to our website visitors and in no way, represent any affiliation or endorsement of the information provided on those linked websites. These links are provided solely for your convenience and to assist you in learning more information on this topic. However, Philips does not control, endorse or guarantee the accuracy of the information contained on the linked sites. In addition, Philips makes no representations or warranties of any kind with regards to any third-party websites or information contained therein. If you have any questions or concerns about the information on the linked third-party websites, please contact the third-party websites directly.



