Skin Changes
Symptom Details
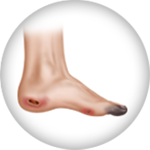
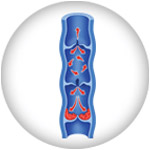
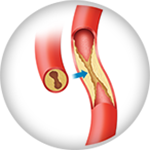
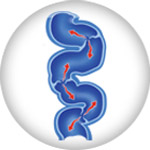
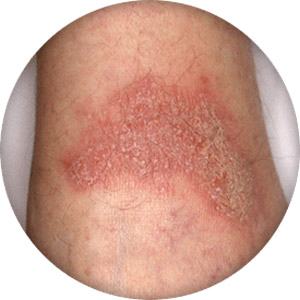
Arterial conditions, such as peripheral artery disease (PAD) and critical limb ischemia (CLI), and venous conditions, such as deep venous disease (DVD) and superficial venous insufficiency (SVI) can produce notable changes in the skin, especially on the legs and feet. Changes in the texture and color of the skin are a result of poor circulation in the arteries and veins.2,3,4 When the circulation is compromised blood flow is decreased resulting in increased pressure in the vessels, leading to inflammation of the skin on one or both legs. The resulting inflammation may cause the skin to become leathery, itchy or reddish.1 Without treatment, increased swelling and skin inflammation due to poor circulation of blood can lead to serious complications such as rash, sores that are open as well as other ulcerations.5 Venous insufficiencies (DVI) can lead to stasis dermatitis which causes itching, scaling, hyperpigmentation, and sometimes ulceration.7 These are serious conditions that require prompt diagnosis and treatment. It is important you take the step and seek help from your doctor if you notice changes in your skin. Skin changes to your feet or legs can be a sign of several conditions such as PAD, DVD or SVI. The progressive conditions may start out with mild symptoms but with time, may lead to more moderate to severe symptoms.
Mild
Moderate
Severe
Causes
When PVD causes skin changes it is a direct result of poor circulation. Trauma or surgery can also cause injury to an artery or vein resulting in skin changes. There are a number of other diseases and conditions not related to PVD that can exhibit skin changes. Only your doctor can pinpoint the cause of your skin changes.
Risk Factors

There are many risk factors that may predispose a person to developing skin changes due to PVD. In addition to vascular causes, other risk factors include:1
What to Look For
Skin Changes
Associated Symptoms
Varicose Veins
Varicose veins can become inflamed when the pooling of blood results in pressure on the vein walls resulting in redness, swelling, and a diffuse pain.
Swelling
Blood pooling in the legs creates pressure on the valves of the veins and damages the capillaries (small blood vessels) and leads to swelling.
Non-Healing Wounds
Ulcers can develop on both the legs and the feet. Ulcers which are above the ankle are usually a result of severe venous disease; the skin breaks down over time and wounds develop. Wounds that won’t heal or are slow to heal on the lower ankle and foot and a result of CLI, where the arteries are unable to bring oxygen rich blood to the foot and the tissues begin to die.
When to See a Doctor
Skin changes and discoloration may be a sign of a condition, such as PAD and DVD, which progresses if not treated properly. Other conditions such as CLI may produce skin changes that require prompt medical attention right away. Talk to your doctor if you are concerned about skin changes. In the case of ulcerations, gangrene or black toes, see your doctor immediately.
Helpful Resources

PVD Doctor
Discussion Guide
Get helpful tips and advice on how to talk to your doctor about a PVD screening.

Patient Brochures
Third-Party Resources
Helpful Websites
Blogs
Apps
A mobile app built by cardiologists, to simplify understanding of most cardiac and peripheral vascular conditions and treatments.
Find a Doctor
If you think you are experiencing skin changes, it is important to get help. Take the step and talk to your doctor, or use our tool below to find a specialist near you.
This tool is not inclusive of all specialists. Consult with your insurance provider to find specialists that are covered within your network.
Are You a Healthcare Professional?
Find out how to register your practice with us.
1. “Statsis Dermatitis.” American Academy of Dermatology. 2017. 2. “Peripheral Vascular Disease.” John Hopkins Medicine. n.d. 3. “What are the signs and symptoms of Peripheral Artery Disease?” National Institutes of Health. U.S. Department of Health and Human Services. n.d. 4. Simon et al. “Peripheral artery disease and intermittent claudication.” University of Maryland Medical Center. May 24, 2012. 5. Eberhardt et al. “Chronic Venous Insufficiency.” Circulation. 2014;130:333-346. July 21, 2014. 7. “Venous ulcers,” Medline Plus. U.S. National Library of Medicine. May 24, 2016. 8. Stasis Dermatitis: merckmanuals.com/professional/dermatologic-disorders/dermatitis/stasis-dermatitis
Disclaimer
The opinions and clinical experiences presented herein are for informational purposes only. Individual results may vary depending on a variety of patient-specific attributes and related factors. Dr. Raghu Kolluri has been compensated by Philips for his services in preparing and providing this material for Philips further use and distribution. We offer links to third-party websites that may be of interest to our website visitors and in no way, represent any affiliation or endorsement of the information provided on those linked websites. These links are provided solely for your convenience and to assist you in learning more information on this topic. However, Philips does not control, endorse or guarantee the accuracy of the information contained on the linked sites. In addition, Philips makes no representations or warranties of any kind with regards to any third-party websites or information contained therein. If you have any questions or concerns about the information on the linked third-party websites, please contact the third-party websites directly.